As technology begins to play a bigger role in healthcare across the board, self-care and self-management are terms you’ll hear with increasing regularity.
As part of this infusion of technology into care, medical devices and mobile applications are set to play an important part of self-management for those suffering from chronic conditions such as diabetes.
Now effecting more than 100 million Americans, diabetes is one of the most common conditions to require regular care and management.
Diabetics’ ability to self-monitor plays a big role in their quality of life. For older adults with diabetes, technology has the power to allow caregivers the ability to monitor their condition more closely and intervene if something isn’t right.
Let’s take a look at some important new technologies that are bound to make a significant impact in the lives of those suffering from diabetes.
Not Your Average Insulin
In an era where everything from your refrigerator to your dog’s collar is being dubbed “smart” for its ability to connect to the internet, collect data and be manipulated by its environment or mobile device, it’s only natural that clinical research teams are looking to create medications that have smart capabilities.
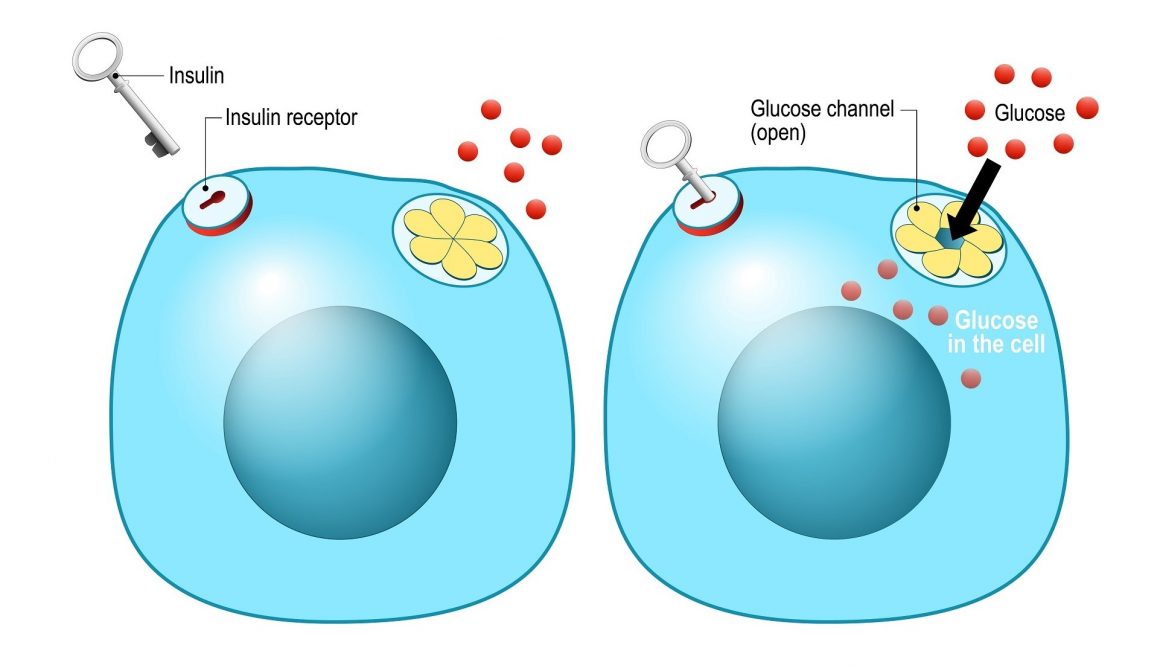
One of these comes in the form of smart insulin, the hormone produced by your pancreas that gives the body the ability to use sugar for energy. This is only an area of research still and has seen researchers fail at attempts at achieving different methods.
The first idea was to modify the insulin molecule so that it would begin to work only when blood glucose levels reached a certain point. The idea actually reached clinical trials, but was found to be ineffective and was eventually abandoned.
Now, more recent research has shifted toward the development of glucose responsive insulin that is engineered biochemically. Designed to bond to the water-soluble protein albumin, these molecules then separate and become active when glucose concentrations increase.
Other methods being researched include insulin which can be inhaled and glucose-responsive insulin delivery via artificial cells which can be implanted or delivered with a patch placed on the skin. While under the skin injections are still the primary method of insulin delivery for diabetics, the need for regular needle insertions may soon change.
Self-Monitoring of Blood Glucose
Continuous monitoring of blood glucose levels is ideal, but has not always been realistic for patients given its cost and the reliability of self-monitoring efforts or medical devices designed to do so. But now, there are several glucose meters on the market which connect by cable or wirelessly to diabetes management programs on computers, smartphones and the cloud.
Health care providers can analyze the date they collect and give feedback to patients as needed. Monitors that do not require a skin prick to read glucose levels have long been a goal and are now available in a number of forms including a glucowatch. In September of 2017, the first continuous glucose monitoring system for adults was approved. It uses a small wire inserted below the skin to serve as a sensor and a wireless mobile reader to show data.
Apps for Diabetics
As you might imagine, there’s a plethora of apps for diabetics, so much so they’re regularly ranked. These can do a variety of functions, from glucose tracking to setting reminders to take medication or tracking weight, caloric intake, blood pressure and glucose levels.
These may be internet based or a mobile download and are quickly proliferating. While research has revealed conflicting reports about their efficacy, one notable study published in the World Journal of Diabetes showed positive results for diabetics who use applications to manage their conditions.
And now, as Alexa and other smart devices make their way into our homes, more applications come with them. Last year, Amazon staged the Alexa Diabetes Challenge to inspire innovators to design Alexa driven solutions for diabetics. The winner was Sugarpod, a creation of Seattle-based Wellpepper which includes a scale, foot scanner and mobile interface to engage patients on a regular basis regarding how they feel while logging vital information.
The scale takes the users weight and then asks if it can take pictures of their feet. It puts those through a machine-learning image classifier designed for the detection of issues such as foot ulcers, a common problem for diabetics. Patients who have these ulcers are at greater risk of amputation.
Additionally, Sugarpod asks users questions and provides diabetes management tips and educational material.
