When you think of biology and microchips, you might think of implants and scenes from movies like The Matrix, Total Recall or The Terminal Man. But while Hollywood loves to tell us stories about the use of microchips inside our bodies, movies don’t show the range of possibilities. One which is currently starting to excite the medical community is the ability of microchips to simulate the human body.
Commonly referred to as organ on a chip technology or human chip technology, microchips lined with living human cells have the potential to change the way that both pharmacological and medical research is done. The hope is that it may drastically alter drug development, personalized medicine and disease modeling while simultaneously presenting a more effective and humane research method than animal testing.
Additionally, chip testing may be more cost effective in the long run and produce more reliable results since animal models often fail to mimic human physiological processes.
How Does It Work?
According to a paper published by researchers at the University of Central Florida in the journal Advanced Functional Materials, “the goal of human‐on‐a‐chip systems is to capture multiorgan complexity and predict the human response to compounds within physiologically relevant platforms.”
In other words, in order for them to understand human reactions to, for example a pharmaceutical compound that could be used in medication, they need something to test it on that more closely mimics the human body’s reactions. This is a necessary precursor to human clinical trials that currently can cost up to $2 billion for the creation of a single compound.
Using cells generally sourced from induced pluripotent stem cells, interdisciplinary teams of computer engineers and medical professionals have designed microdevices capable of recreating the architecture and function of organs such as the lungs, kidneys, skin, intestines, bone marrow and the blood brain barrier.
Scientists are building different organ components and connecting them on a single transparent chip, emulating how these organs connect in the body. The chip is made from a flexible polymer and is around the same size as a memory stick for a computer. It contains channels that are lined with organ specific cells that interface with an environment of artificial veins which facilitate cell fluidity and help mimic living organs when mechanical forces are applied.
Being translucent, they provide a glimpse into the machinations of organ cell activity that scientists have never seen before.
How Far Along is the Research?
The UCF project isn’t the only group looking at this. Harvard’s Wyss Institute for Biologically Inspired Engineering is also working extensively with Human on a Chip technology, focusing on the interconnectedness of organs within the body.
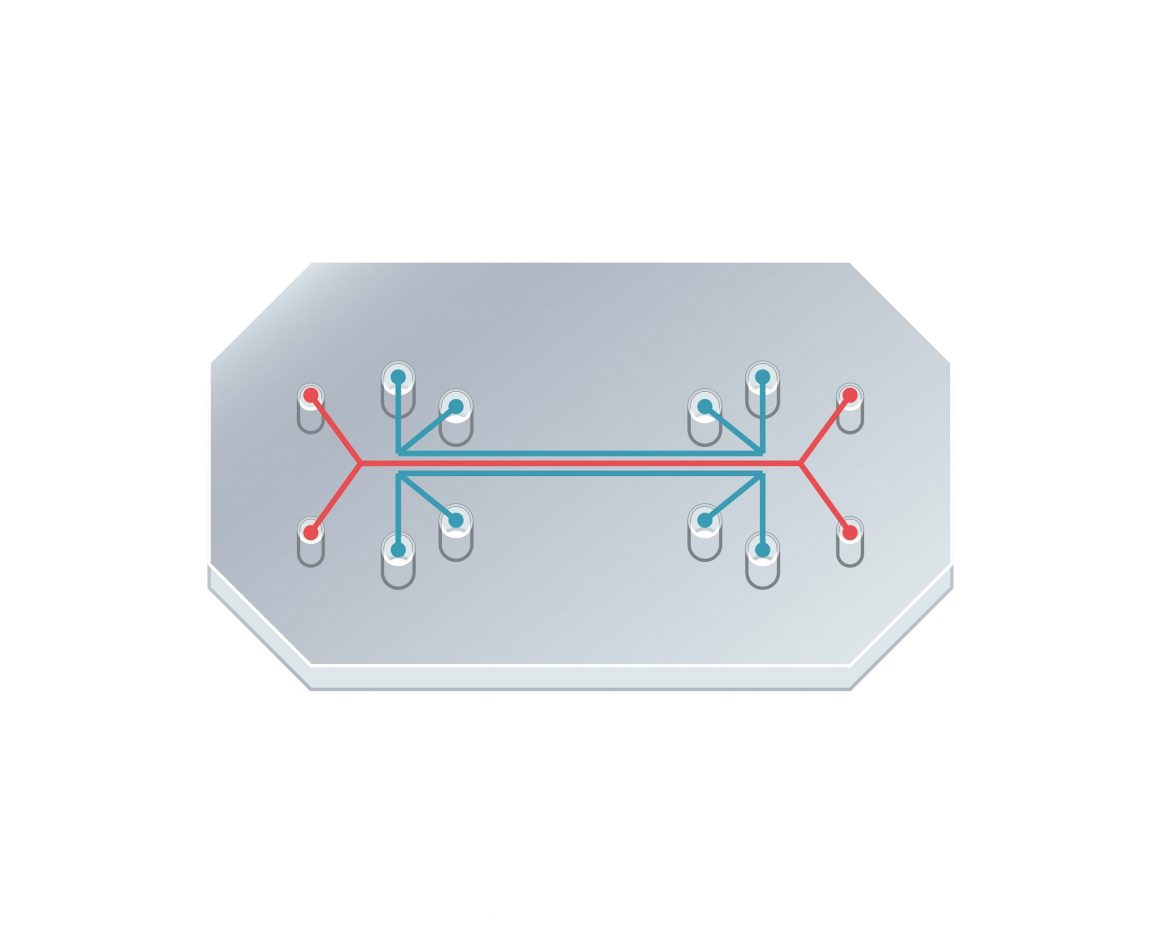
They’ve developed automated methods of transferring fluids through a common vascular network. This allows for real time observations of tissues and the analysis of the responses of ten different organs.
When it comes to aging, the human body ages in a significantly different way from any other species. If researchers can recreate human organs at varying stages of the aging process, they can better attempt to develop treatments and better understand conditions that commonly effect older adults.
The Harvard-based contingent is now working toward the development of human disease models and computer platforms that can help identify new therapies as well as biomarkers. They also hope their work will spur vaccine development and are exploring using it to support personalized medicine efforts by engineering stem cells that are more versatile than the ones used on the chips.
Essentially, the system that supports this research consists of the chips themselves, a computerized research system and software applications that help with the analysis of data and the mechanics of the technology. The Food and Drug Administration has now entered multiyear research and development agreements to evaluate the technology.