Chronic conditions are defined as those that are persistent, have long lasting effects and often get worse with time. They have become a significant issue in American healthcare with their ability to negatively impact a variety of vital organs. Most seem to have one thing in common; they cause damage to the brain.
Chronic conditions affect more than 85% of older adults, according to the National Institutes on Aging, while at least 60% report have more than one condition. This increases the risk of older adults developing neurodegenerative conditions such as dementia and Alzheimer’s Disease.
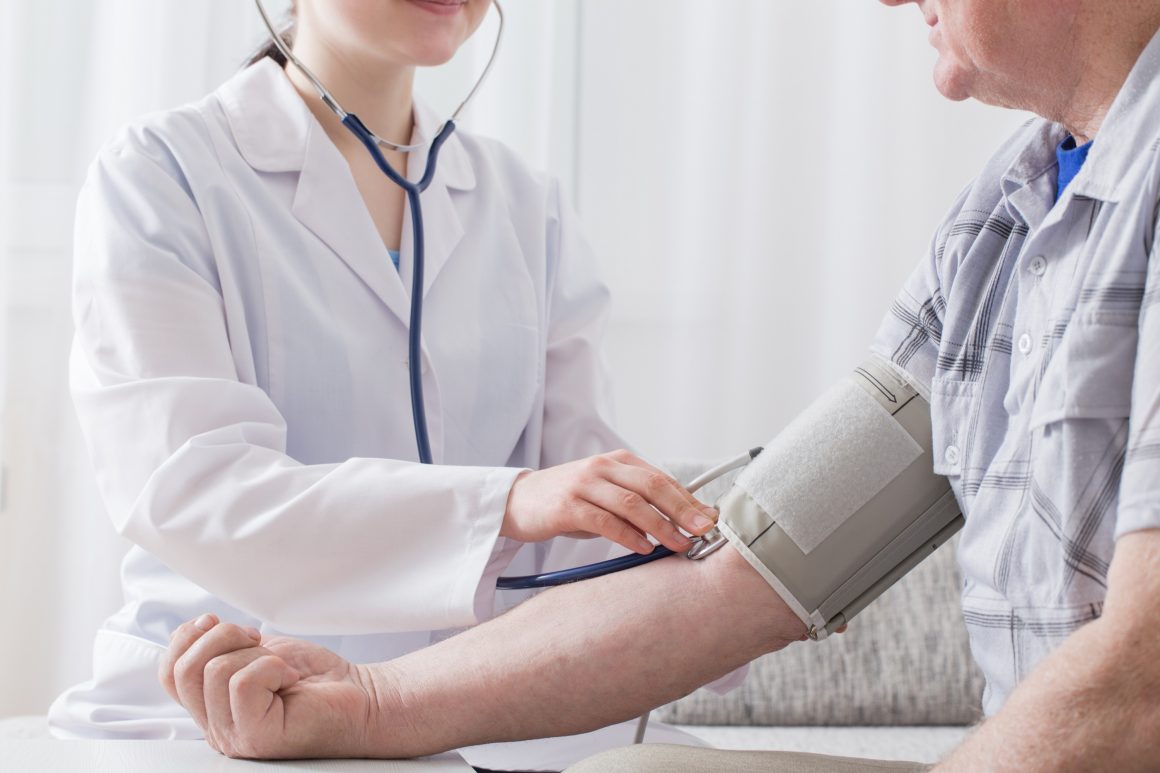
Two of the most well-known examples of this occur in diabetes and hypertension. A study published in The Journal of Nursing Research unveiled that compared with community dwelling older adults with other chronic diseases, the population with hypertension and diabetes had significantly more memory loss and poorer executive function.
Hypertension, especially in midlife, has proven to be a risk factor for cerebral atrophy, damaged white matter and disease in the brain’s blood vessels. Research published in the journal Current Hypertension Reports shows that hypertension fuels the development and progression of neurological changes by “promoting vessel wall remodeling and endothelial dysfunction,” thus increasing the likelihood of developing neurological conditions in old age.
Here are some other chronic conditions that are common in elderly populations and the ways that they speed the development of cognitive decline.
COPD
Chronic obstructive pulmonary disease is the third leading cause of death in the United States, but its effects reach beyond the lungs and into cognition.
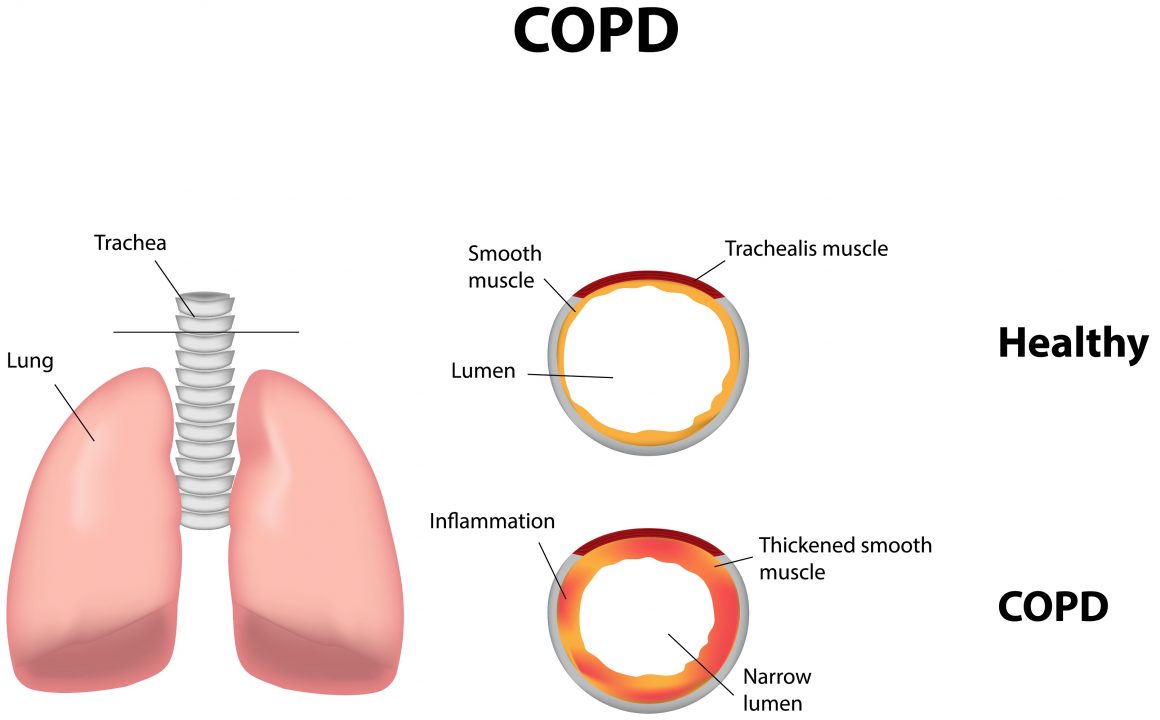
A study published in the journal JAMA Neurology concluded that the restriction of air flow into the body caused by COPD increases the risk of developing mild cognitive impairment by 83%. Other studies have revealed that COPD is associated with poor performance on tests of attention, memory, and executive function.
Depression
A common condition across populations, depression is something that damages cognitive function, even when participants are given medication to treat it. Current depression medications typically address issues related to emotional function, but have done little to enhance cognition, according to research published in The Lancet which looked at the effect of antidepressants on cognitive impairment associated with depression.
The fact is depression causes major lifestyle changes that affect your natural rhythms and damage the ability to think clearly. Examples of this include loss of energy and interest in things that are typically enjoyable and sleeping or eating too much or too little.
Chronic Kidney Disease
The link between kidney dysfunction and cognitive impairment has long been established, but what was once known as “dialysis dementia” has been found to be present even in early stage chronic kidney disease (CKD) patients, according to a study published in the journal Nephrology Dialysis Transplantation.
CKD can cause dementia that is not age related, but it can also worsen the condition of older adults already prone to cognitive decline. One reason is that decreases the kidneys glomerular filtration rate (GFR), or in other words, the level at which the kidneys function. The lower GFR a person has, the greater their risk of experiencing cognitive decline due to CKD.
One reason for this is that current CKD treatments such as dialysis do little to stop the advancement of cognitive decline, leading experts believe that the clearance of toxins, uncontrolled thyroid conditions and anemia could be supporting the development of cognitive impairment.
